|
Sensory Modulation Disorder  Sensory Modulation Disorder is one specific type of Sensory Processing Disorder (SPD). Sensory modulation refers specifically to the brain’s ability to respond appropriately to the sensory environment and to remain at the appropriate level of arousal or alertness. There are three primary types of Sensory Modulation Disorder. Over-Responsivity: An exaggerated response of the nervous system to sensory input. For example, people who get motion sick easily are over-responding to vestibular input (the sensation of movement). The nervous system goes into fight-or-flight mode even when no real danger exists. Under-Responsivity: A lack of response, or insufficient response to the sensory environment. Sometimes these people appear to be daydreaming or unfocused on what is happening around them. They may also be uncoordinated and have difficulty with motor skills development. Sensory-seeking: The nervous system of the sensory-seeker needs intense input in order for the sensation to be registered properly in the brain. Therefore the sensory-seeker craves intense sensations constantly. Symptoms of Over-Responsivity include:
 Symptoms of Under-Responsivity include:
Symptoms of Sensory-seeking include:
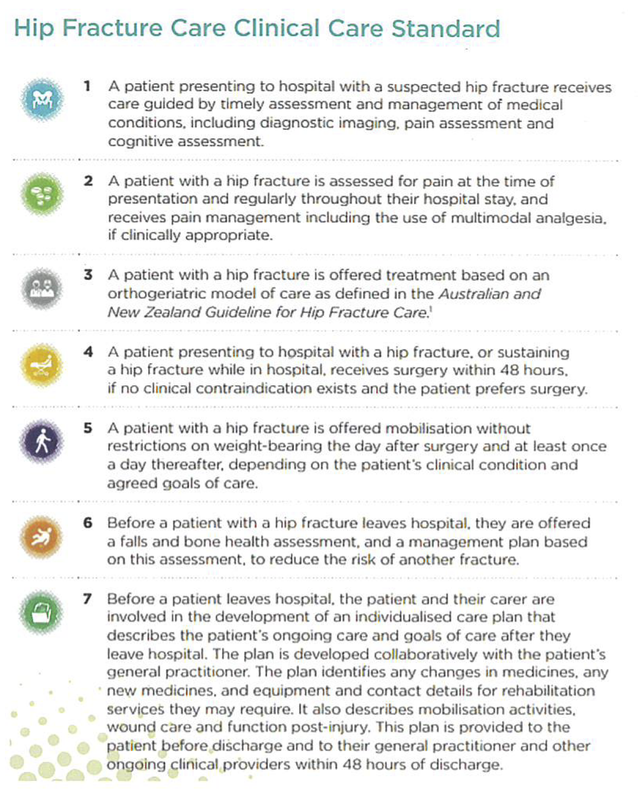
If you feel like you or your child may have some of these symptoms which are interfering with your / their quality of life, our occupational therapists can help you. They will identify and give you strategies to manage yours or your child’s sensory issues. You don’t have to struggle alone, just call us at Therapy Professionals Ltd Phone: 03 377 5280 Email: [email protected] Hip Fracture Care Working together to improve outcomes One in two people don’t return to their usual level of working within the first year and one in four people aren’t alive a year after their fall Australian and New Zealand Hip Fracture Registry Aged Care NZ Issue 01 2022 If you have ever broken your hip or cared for someone who has, you will know the significant impact this injury can have on wellbeing and independence. Whether falling from a loss of balance when turning, a misstep on an unexpected foot path or a topple off a step stool, the result can be the same – a hip fracture. Unfortunately this happens to almost 4000 New Zealanders a year. Although there are excellent medications to deal with pain and operations to put bones back together, not everyone makes a full recovery. One in two people don’t return to their usual level of walking within the first year and one in four aren’t alive a year after their fall.  The Australian and New Zealand Hip Fracture Registry (ANZHFR) was established in 2013 with the aim to improve the care and outcomes for patients who have a hip fracture. The Registry achieves this by collecting data about older people admitted to hospital with a fractured hip and making this information easily available to clinicians, patients and their families. The Registry also provides education to clinicians about best practice for hip fracture care and encourages research to understand what contributes to a successful outcome. The Hip Fracture Registry is run by a group of committed clinicians and researchers who come from a range of specialties and organisations involved in hip fracture care and bone health. This multi-disciplinary approach and teamwork is a hallmark of providing best practice hip fracture care. In New Zealand, every hospital that does hip fracture repair surgery has been approved by local ethics committee to contribute data to the Registry. In practice, each hospital has a nominated nurse or doctor who provides patients with an information sheet and then collects relevant information from the hospital records and enters this into the registry database. Patients can request to ‘opt off’ if they wish. This data allows hospitals to audit the care they provide against key markers of safe, high-quality care called clinical standards. There are seven Hip Fracture Clinical Care Standards (see below) which include timely assessment, appropriate pain management, involvement of Geriatricians (specialists in the care of older people), providing support to walk the day after surgery, assessment and management of falls and bone health and planning for discharge. This data can be used to improve clinical performance, advocate for better clinical care and ultimately improve the recovery for patients. Information on how well hospitals are meeting Clinical Care Standards is available for all to see on the registry website www.anzfr.org and in an annual report published each September International evidence shows that registries that are well run do improve care for patients. Since the first hospitals in New Zealand joined the Registry in 2015, we have seen steady improvement in several important areas. More patients are receiving a nerve block to help manage their pain when they first present to medical care, most patients are having their hip operation within 48 hours and more people are being supported to get up and walk the day after their operation. Hip fracture care involves a large number of different specialists and clinicians including emergency department doctors and nurses, anaesthetists, orthopaedic surgeons, geriatricians, orthopaedic nurses and therapists. We have seen that the hospitals that have been able to make the most improvements are those when the whole team is on the same page and providing well-coordinated care. It takes a great deal of work, persistence and energy to achieve this level of co-ordination and improvement. In 2021 the Registry recognised the best performing hospital across all the areas of hip fracture care by awarding our first ever Golden Hip award. This went to North Shore hospital who are leading the way in many aspects of the coordination of their care. The Registry recognises that people who have had an experience of breaking their hip are in a valuable position to provide feedback and advice about future areas to improve. Our consumer representative plays a key role in telling the patient story and sharing the challenges of being a patient. With the support of the Health Quality and Safety Commission (HQSC), a workshop was held in 2020 with consumers to understand more about their experiences while in hospital. Following this workshop, the Hip Fracture Care Guide was developed to provide patients and their families information about what happened during the hospital stay and advice for ongoing recovery back in the community. This guide is available on the HQSC website. Our next focus of work is to consider how to collect information about outcomes that are important to patients. These are commonly known as Patient Reported Outcome Measures (PROM) and include aspects important to patients such as being independent and healthy. The Registry now has over 16,000 New Zealand records that provides a wealth of information to use for research. We are very grateful to the patients who allow this information to be collected so we can continue to identify key aspects of care which will make a positive difference to how people recover. We are currently using the data we have to review whether different types of operations result in different outcomes, whether having cognitive impairment makes a difference to recovery and whether Covid-19 has had any impact on the care people have had in hospital. All the people involved in the ANZHFR will continue to work hard to improve the outcomes for patients once they have broken their hip. However, our golden wish would be that less people experience this potentially devastating injury. Prevention is definitely better than treatment, which is why the ANZHFR fully supports the ongoing focus on falls prevention programmes such as Live Stronger for Longer and the work by Osteoporosis NZ on bone health. Ref: Aged Care NZ, Aged Care NZ Issue 01 2022
It’s time… A daily routine is important for all people but it is particularly important for seniors.  Young or old, people are most afraid of the unknown. And as some lose control over their physical abilities, independence, or cognitive abilities, their world becomes filled with more and more unknowns, and if their days are unstructured and unpredictable, that can add more stress. That’s why having a regular daily routine helps both seniors and caregivers. Everyone knows what to expect and there’s no need to think or worry about what will happen next. Following a daily routine can reduce stress, increase the feeling of security and improve sleep. What is a daily routine? A routine means doing the same basic activities around the same time every day. This gives structure and a natural flow to the day. Having a routine also makes it easier to remember if the older adult has done necessary things like take medicine, use the bathroom, drink water, and eat. For example, part of a regular daily routine would be to wake up at 8 am, use the toilet, brush teeth, wash face, comb hair, change from pyjamas to regular clothes, then sit down to a hot breakfast of oatmeal and coffee. After that, the older adult would take their morning medications. When one creates a daily routine for an older adult, it should ideally be based roughly on their current daily activities so the adjustment isn’t too difficult. In addition, keep in mind that a rigid schedule is not necessary.  It makes the transition to home care easier When a senior accepts outside help, it can be difficult in the beginning to get used to having a new person in their life, especially now that the person providing care is taking on responsibilities that the senior used to do in the past. Reduced stress and anxiety Seniors who no longer have control over their lives may feel constantly stressed and anxious. They may feel disoriented or unsure about what’s going to happen in the next moment. This often happens when someone has Alzheimer’s, dementia, stroke or other health conditions that causes significant cognitive or physical impairment  Some older adults may have become too ill or frail to manage their days; they’re dependent on others for all the usual tasks of daily living. And when they’re so dependent, not knowing when or if their needs will be met is another source of stress. A predictable routine reduces stress and anxiety because seniors know exactly what will be happening, who will be helping them, how the activity will be done, and when it will occur. Over time, these routine actions will become part of their body memory. They won’t have to consciously think or worry about what’s coming next. Stop the power struggles Most people dislike being told what to do and when to do it and seniors are no exception. But if an older adult has a consistent daily or weekly routine, the activity is simply what’s done at that time (getting dressed, eating, bathing etc). Once a routine becomes a natural part of their life, they will be more likely to go with the flow of activities and won’t feel like you’re suddenly forcing them to do a certain activity. Increased co-operation Nobody likes disruption. When a carer and older adult both know what's going to happen and when, there is less stress and uncertainty in their lives. And when someone can anticipate the next task or activity, they can mentally prepare and will be more willing to participate than if they feel surprised by a seemingly random activity. Even if the older adult has dementia, their subconscious can develop a sense for the regular rhythm of the day. That helps them feel more comfortable and secure even if they aren’t outwardly aware of the routine. Reduce the need for decision-making Making decisions all day is tiring, even if they’re minor ones. A regular daily routine saves valuable mental energy because most of the tasks, timing and activities have already been decided. This significantly reduces the number of choices needed so energy can be spent on other things.  Improves sleep quality Having a regular daily routine also helps older adults sleep better. A study found that doing the same basic activities such has eating, dressing, and bathing at the same time every day improves sleep quality. Since many older adults have trouble sleeping through the night, creating a regular daily routine is a simple, non-drug way to improve the situation. Seniors, especially those with dementia and other cognitive impairments, have lower quality sleep. However, scientific studies now show that a daily routine results in better quality sleep, both by promoting a deeper sleep as well as a lengthier one. Quality sleep can improve mood and allow people to deal with events in their day in a much more positive manner than if they were sleep deprived. Build in time to enjoy each other With all the responsibilities of care giving, spending quality time with an older adult often gets pushed to the bottom of the ‘to do’ list. Make it easier to spend quality time together by building it into their daily, weekly or monthly routine. It could be as simple as starting each morning with a hug, ending the day with a bedtime song, enjoying a nice walk in the park every Sunday afternoon, or having lunch at their favourite restaurant once a month. From Aged Care NZ Issue 01 2022 Hip Care Tips for six weeks after your operation 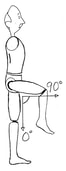 Do nots: · Don’t bend your hip more than 90º · Don’t sit or lie with your legs crossed at the knees or ankles · Don’t jar or force movements at the hip · Don’t swivel or twist affected leg · Don’t put pressure on the wound · Don’t put weight on your operated leg for long periods · Don’t bend forward when getting on and off sitting surfaces 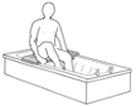 The Bath Avoid sitting in the bath for the first six - eight weeks. If you do not have a shower we will order a bath board for you and you will be instructed how to get in and out of the bath. 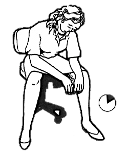 Showering We can arrange for you to have a high shower stool in order to take weight off the operated leg and to reduce the chance of falling.  Dressing
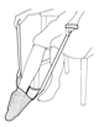 Use aids from your long handled kit to avoid bending eg
Elastic shoe laces are available.  The Bed
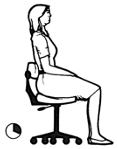
 Sitting
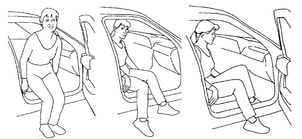 The car Follow your surgeon’s advice about driving To get into a car put your bottom on the seat and swing your feet into the car. To get out of car swing legs out gently and then stand up holding onto stabilised car door Stairs NB Good leg (leads) up to heaven. Bad leg (leads down) to hell.
Sports/Hobbies Check with your surgeon before restarting active sports or hobbies ie cycling, gardening, bowls. Sexual Activity Ensure any sexual activity does not place any strain on your operated hip and that your hip doesn’t bend greater than 90º for at least three months post-operatively. Home Help If you require assistance with meal preparation and/or home help ask your hospital nurse. |
AuthorShonagh O'Hagan Archives
July 2024
|


 RSS Feed
RSS Feed