|
Leaky water works - Incontinence  There are many myths about incontinence, which are not necessarily true. For instance many people believe incontinence is an inevitable consequence of ageing or if you drink less it will improve the problem. Neither of these beliefs is helpful. Some facts about our Water Works:
There are two types of incontinence – Stress and Urgency.  Stress incontinence With stress incontinence there may be leaking when coughing, sneezing, jumping, lifting, pushing, laughing and pulling. This is caused by weak pelvic floor and urethra sphincter muscles. The trick is to strengthen your pelvic floor and urethral sphincter muscles and tighten your pelvic floor muscles before stressful activity occurs. Urgency incontinence Urgency incontinence is the sudden need to go, for example, when opening the front door you generally get the urge. It’s caused by an overactive bladder, which has been trained to empty before it’s full. Typically small amounts of urine are passed more frequently -10 plus times a day. Preventing or fixing incontinence For both types of incontinence strengthening your pelvic floor and urethra sphincter are important. To do this:
Tips for managing and training urgency incontinence When you experience the sudden urgency to pass urine, it is often associated with a feeling of panic. The following may help:
If desperate:
If you are still struggling there is help:
You don’t have to suffer alone - contact us we can help
Ph: 03 3775280 Email: [email protected] Web: www.therapyprofessionals.co.nz Reference: Women’s Waterworks – Curing Incontinence by Pauline E Chiarelli New guidelines for provision of physiotherapy in aged care in New Zealand Providing the best care for older people living in ARC, who have diverse functional abilities, health needs and cognitive function is challenging from Aged Care New Zealand Issue 1 2022  Physiotherapy New Zealand (PNZ) is soon to release the first NZ guidelines for Aged Residential Care (ARC) managers on the benefits and utilisation of physiotherapy services in ARC, developed by members of the Physiotherapy for the Older Adult Special Interest Group of PNZ. The provision of physiotherapy services in ARC has long been unclear with the contractual requirements being ‘grey’ at best. These guidelines aim to provide managers with information around the immense benefits of a robust and effective physiotherapy service, and the ‘how to’ of selecting and planning high quality physiotherapy services for their residents. Mobility and independent function are highly valued by older people and their whanau and are essential to the wellbeing and health related quality of life of older people. Aged Residential Care is a vital part of our health system where over 50 percent of all individuals will stay for some of their lives. Some people will live in ARC for up to five years or longer, and those years spent living in ARC, can be a very meaningful experience for an older person. Providing the best care for older people living in ARC, who have diverse functional abilities, health needs, and cognitive function, is challenging. Utilising physiotherapy allows facilities to support their resident’s physical functioning, enable their well-being, rehabilitate them from injury and illness, manage long term conditions, and delay the onset of frailty and disability. The newly developed guidelines include:
These guidelines have been needed for many years. A report to Physiotherapy New Zealand on physiotherapy services. The report outlined inadequate provision of physiotherapy service and examples of physiotherapy assistants working without supervision of a physiotherapist. In 2022 physiotherapists see extreme variation in the provision of physiotherapy, ranging from 20 ᐩ hours per week right down to hospital level care facilities with no weekly physiotherapy provision. The urgency for these guidelines was highlighted in the initial response to Covid 19 when New Zealand moved to Alert levels 3 and 4 in 2020 and the country went into lockdown. Huge variation in access to physiotherapy services was seen across the country. Although many facilities engaged with telehealth there were some ARC facilities who did not engage with physiotherapy services at all. On the return of physiotherapy services to facilities there were numerous cases of irreversible loss of mobility and function in residents over the two-month period. These guidelines will not just inform managers but will also be an essential guideline allowing more informed consumers to ask appropriate questions when selecting their ARC facility. Generally, physiotherapy services are listed on Eldernet as “yes/no” with limited information on the physiotherapy services provided. These guidelines will give consumers the understanding to ask detailed questions about hours of physiotherapy each week, what can be expected in terms of assessment and input for themselves or their whanau and allow them to understand how the provision of a robust physiotherapy service can improve their experience of ARC living. Ref: Aged Care NZ, Issue 01 2022 Physiotherapy NZ Older Adult If you are interested in receiving a copy of these guidelines when they are released, please contact [email protected] Therapy Professionals Ltd, Christchurch, NZ has been supplying physiotherapy services since 1985. We understand the needs of the residents, staff and facility.
Phone: 03 377 5280 Email: [email protected] Conscious activity prevents muscle loss Muscle loss might be an inevitable part of ageing, but exercise can slow the process down. From: Aged Care New Zealand Issue 02 2021  Here’s a sobering fact: one can lose up to 40 percent of muscle mass between your 20s and 80s. That might sound outlandish, but it’s a natural part of ageing. Known as sarcopenia, this is a gradual loss of muscle mass that occurs as we age. Although we can start losing muscles from our 20s, this loss really speeds up once we hit our 60s. At the same time that sarcopenia causes loss of muscle mass, we simultaneously gain fat mass, and see a big drop in strength too. All of this can have a big impact on how well an older person moves. Muscle mass plays a huge role in our health. So much so that sarcopenia and sarcopenic obesity (the combination of low muscle mass and excess fat), and dynapenia (the loss of muscle strength) are associated with a surprisingly wide range of health conditions, from heart disease and diabetes to frailty and dementia. In fact, in people who already have heart disease, those with the highest levels of muscle mass seem to have the best chance of living longer. On the other hand, people with the lowest amounts of muscle seem to be at highest risk of dying prematurely from all causes. This tells us that muscle might play a protective role in heart health. Why this happens, we don’t yet know – but it may have something to do with chemical messengers (myokines) produce by healthy muscles, which can help reduce inflammation throughout the body. Another major benefit of having healthy muscles is that they help protect us from diabetes, which can help reduce inflammation throughout the body. When we eat and digest carbohydrates - such as potatoes, bread or rice – sugar enters our blood stream, a lot of which is sent to our muscles. Our muscles use this sugar for energy or store it as glycogen in order to maintain stable blood sugar levels. This process is an important part of blood sugar control and explains why people with less muscle are more likely to develop diabetes. In older people, low levels of muscle are also linked with a great frailty, weakness, and being less able to carry out normal daily activities. This means people can have trouble with regular tasks such as getting out of bed, standing up from chairs, climbing the stairs or carrying groceries. All of this can make living independently a lot more difficult. Difficulty moving can also mean people end up moving even less which speeds up muscle loss. People with sarcopenia who lead sedentary lives are also at greater risk of osteoporosis. This is because active muscles send signals to bones that help them stay strong. The drop in strength from sarcopenia means people may be more prone to falls and bone fractures. Again, this fear of falling may make some people more sedentary, which may reduce quality of life and put them at a greater risk of depression  Although sarcopenia is a natural part of ageing, muscle loss is largely accelerated by inactivity. As we get older, we tend to move less. But exercise is one of the key signals that our body needs to keep our muscles strong and healthy. Without that signal our muscles start getting smaller and weaker over time. Eating protein also acts as a signal to grow and maintain muscle. However, as we age, we tend to have smaller appetites and eat less protein, increasing the risk of muscle loss. Lower levels of the hormones, testosterone and oestrogen, higher levels of fat, insulin resistance (where the body doesn’t handle glucose as it should, which can lead to diabetes) and higher levels of inflammation are other reasons why older people lose muscle more easily than younger people. In fact, all of these factors combined lead to something called “anabolic resistance”. This means the body doesn’t respond as well to the signals that normally cause muscles to grow. If that isn't enough, current COVID-19 restrictions may be making muscle loss even more likely. Data from smartphones has shown that people have been more sedentary than usual during lockdown. We also know that people’s sleep quality has declined, and people are probably feeling more stress and anxiety. These factors can also speed up muscle loss by affecting hormones that increase muscle breakdown and encourage weight gain by affecting appetite hormones, causing people to eat more processed foods that have more calories. This is called a ‘catabolic crisis’ – a brief period of time when conditions come together to make muscle loss much more likely. Another example of a catabolic crisis would be if someone was hospitalised or forced to spend days, or even weeks in bed. COVID-19 could very well create a catabolic crisis for many adults after lockdown.  Muscle loss can be prevented – or at least slowed – with a few lifestyle changes, namely exercise activity and diet. Resistance exercise, such as lifting light weights or using elastic resistance bands, helps keep muscles strong and healthy and regular walking can help too. High protein diets, containing foods such as lean meats, fish, eggs and low-fat dairy products can also help to build and maintain more muscle than exercise alone. Getting at least 25-40 grams of protein each meal is especially important. On top of that, widely available supplements including Vitamin D, fish oil and creatine (a naturally occurring substance found in the muscles which helps them produce energy) may help people hold on to more muscle and improve their quality of life as they age. During the pandemic, when muscle loss is more likely, prioritising regular exercise and a healthy diet can make a big difference to long-term health. Authors:
Richard Kirwin, PhD Researcher Clinical Nutrition and Physiology, Liverpool John Moores University and Claire Stewart, Professor of Stem Cell Biology, Liverpool John Moores University. From: Aged Care NZ Issue 02 2021 Here at Therapy Professionals Ltd our friendly therapists can assist you to improve your diet and exercise to slow down the loss of your muscle bulk. Just phone: 03 377 5280 or email us at [email protected] Seating people comfortably 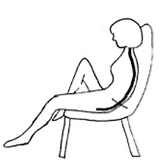 Many elderly and disabled people in care sit for long periods of time. Some are able to move themselves while others are not able to move without assistance. For those of us caring for the elderly and disabled we need to think carefully about how we seat those in our care. We need to consider things like:
Good posture is important to prevent back pain, encourage mobility, assist swallowing and prevent chest infections. When choosing a chair for a client it needs to be supportive to prevent them from slumping over. When sitting for long periods of time without being able to adjust your position, circulation to areas on a person’s bottom, legs and back can be cut off causing discomfort and, if left, pressure sores.  Pressure relief is important. Some chairs have pressure relief features built into them; we recommend these, especially for people who are unable to change their position. Alternatively pressure cushions can be used. Air filled pressure cushions (Rohos) can be problematic. They can be slippery causing a person to slide forward into a slumped posture. A slumped posture is uncomfortable, can make it hard to swallow and breathe effectively and take part in activities. The cushions raise the height of the seat, which may cause the feet to dangle, leading to discomfort under the thighs. While sitting it’s important to have feet on the floor or a footrest. 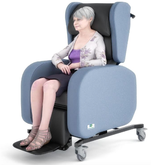 For more information on pressure injuries follow this link. https://www.therapyprofessionals.co.nz/uploads/4/9/5/2/49523375/skin_injuries_caused_by_pressure.pdf Keeping people mobile as long as possible is in everyone’s best interests. If you are caring for someone who can still stand themselves up or better still walk safely, it’s important you choose a seat that encourages them to stand and get out of easily. This means their feet must be flat on the floor, the chair has armrests at the right height to push up from and the seat surface is firm enough to wriggle forward. The ideal seat for a person, maintains an upright posture with their bottom back in the chair and hips at a 90 degree angle. The chair needs to support the spine, thighs with a gap behind the knees and the armrests should support the arms with relaxed shoulders. Feet need to be flat on the floor or supported on a footstool. For more information on choosing a seat follow this link https://www.therapyprofessionals.co.nz/uploads/4/9/5/2/49523375/choosing_a_comfy_armchair__.pdf If you need some help seating the elderly or disabled in your care our friendly Physiotherapists and Occupational Therapists can help just contact us at Therapy Professionals. Ph: 03 3775280 Email: [email protected] |
AuthorShonagh O'Hagan Archives
July 2024
|

 RSS Feed
RSS Feed