 Maintaining skin health in older people Age related changes in the skin mean older people are of increased risk of skin breakdown, and should be supported to maintain good skin health. This article examines general skincare for older people, skin barrier function and the skin changes associated with the ageing process. Skin assessment and the use of washing products and emollients are discussed and methods by which older people and nursing staff can help to promote and improve skin health are identified. As the skin ages it becomes less able to perform its key barrier functions and skin breakdown becomes an increasing risk. This can have a detrimental impact on quality of life with major economic implications (Gardiner, et al 2008), so skin health is essential to the wellbeing of older people and a central component of nursing care. It is estimated that approximately 70 per cent of older people in Australia experience skin problems, many of which are preventable. Structure and function of the skin The skin is the largest organ of the body, covering approximately two square metres (Penzer and Ersser, 2010). It performs a number of functions including:
The skin has two main layers: the epidermis (outer layer) and the dermis. These provide supportive structures allowing the epidermis to function. The stratum corneum provides the skin barrier. In normal skin it is resilient, protecting the underlying skin from the penetration of irritants and allergens and preventing the loss of wafer from the body. The corneocytes are full of water; this results in a smooth barrier with no cracking between the corneocytes, which also contain high levels of natural moisturising factor (NMF) -a humectant. Normal skin is smooth and elastic and does not itch (Cork and Danby, 2009). The natural pH of the skin is slightly acidic – between 4 and 5.5 – providing protection from microbes (Cowdell, 2010). Damage to the skin barrier allows for water to be lost and irritants and allergens to be introduced, leading to inflammation (Cork et al, 2006). 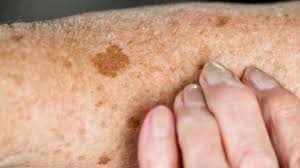 Skin ageing As we age the skin is affected both by intrinsic and extrinsic factors. Intrinsic ageing is the ‘programmed’ true biological changes (Lawton, 2007). Extrinsic factors, such as damage from exposure to the environment (Lawton, 2007) and the sun (ultraviolet exposure) also affect skin ageing. Other extrinsic factors include smoking, environmental pollutants (Lawton, 2007), reduced peripheral sensation, reduced mobility, incontinence, depression and dementia, polypharmacy, diabetes and vascular changes and poor nutrition (Finch, 2003). Although ageing cannot be prevented, strategies to enhance skin-barrier function can be used and the risk associated with extrinsic factors can be reduced. It is estimated than at least 70 per cent of older people will have a skin problem (APGS, 2000) and skin conditions are on the most common reasons for primary care consultations (Schofield et al, 2011). Davies (2008) identified skin conditions that commonly affect older people (Kirkup, 2006) possibly because they see skin deterioration as an inevitable part of ageing and believe no help is available. Fanos and Laird (2001) also noted that clinicians may see concerns as trivial. It is therefore important that nurses routinely enquire about skin heath in older people and undertake accurate and thorough skin assessment to identify problems (Nazarko, 2009). Assessment is not a one-off activity but an ongoing process, involving monitoring change and response to treatment. It should include:
Finch (2003) gave a detailed explanation of skin assessment. If any skin problems are identified on general assessment, further assessment, investigation, and completion of risk assessment tools should be undertaken as required. Skin Care Skin care is one of the cornerstones of nursing practice, but the importance of general skin care is an area of practice that is often overlooked (Castledine, 2003). However, maintaining or improving skin health is generally neither costly nor difficult. Simple, low-cost interventions can have a positive impact on quality of life and help to prevent skin breakdown. Skin hygiene is essential for skin health and important in promoting personal wellbeing. For older people with dry skin, it is particularly important to achieve a balance between cleanliness and over washing, which may damage the barrier function (Voegell, 2008a). Use of appropriate washing products and emollients can contribute to maintaining skin health. Washing products Washing with soap and water remains the standard method of skin cleansing (Ersser et al, 2005) and is recommended in many nursing texts (for example, Downey and Lloyd, 2008; Dougherty and Lister, 2008). However this can cause an increase in skin pH (Korting et al, 1987), which can alter the skin’s normal bacterial flora, increasing the like hood of colonisation with more pathogenic organisms (Cooper and Gray, 2001). The increase in pH can also damage the skin barrier and cause irritation (Kirsner and Froelich, 1998). Soap also removes lipids from the surface of the skin and over washing removes NMF (Pe ters, 2001), resulting in further skin dryness. If acceptable to the individual, using emollient and soap-substitute products rather than soap will help to maintain skin health. Emollients Emollients increase the amount of water held in the stratum corneum, either by occlusion (trapping the water in and preventing evaporation), or by actively drawing water into the stratum corneum from the dermis (Ersser et al, 2009). They play a crucial but often undervalued role in skin health and are the mainstay of therapeutic treatment for older patients with dry and itchy skin. Although their benefits are widely acknowledged in the field of dermatology, they have tended to be undervalued and underused in general care (Lawton, 2010). Adverse effects from emollients are rare, although occasionally sensitisation to an ingredient may occur. There are many formulations of topical emollients including ointments, creams, lotions, gels and sprays. Ointments are the greasiest preparations and often contain paraffin; creams are an emulsion of oil and water; lotions are the least greasy, making them less effective as an emollient. Cosmetic acceptability is, however, an important consideration. Some products contain humectants such as urea or lipids (NMF), which provide excellent moisturisation (Lawton, 2010). Emollients alone may be sufficient to alleviate skin dryness but can be considered as adjuvant therapy alongside other tropical or systemic treatments in chronic skin conditions such as eczema or psoriasis (Ersser et al, 2009). There is little scientific evidence on how to apply emollients, although it is generally agreed they should be applied using a gentle stroking motion following the lie of the hair on the body (Penzer and Ersser, 2010). This rationale is based on the principle that rubbing with a greasy emollient may lead to an irritated or blocked hair follicle and subsequent folliculitis. Ersser et al (2009) recommend application of emollients during the day at times convenient to the individual – this may be as frequently as every two to three hours, and at bedtime. A greasier emollient may be acceptable for use overnight, so it is important that an adequate supply and several preparations are available.  Self-care Self-care and self-management are central to Australian health policies and undoubtedly the majority or older people would prefer to meet their own skin-care needs as far as they are able. Nurses should facilitate self-care wherever possible to ensure effective skin care and minimise deterioration in condition (Burr, 2007). Many older people can care for their own skin provided they have sufficient knowledge, skills and confidence to do this (Bandura, 1997). They may face difficulties such as reduced mobility and dexterity, cognitive impairment, increased frailty and difficult social circumstances but these can often be minimised or overcome if the multidisciplinary team is involved, and they are advised on different techniques or enabled to use appropriate aids. Conclusion Skin health is essential to the wellbeing of older people and a fundamental aspect of nursing care. Nurses should regularly assess the skin health of older patients, promote self-care and encourage the use of appropriate products. Authors: Fiona Cowdell, senior research fellow and graduate research director at the Faculty of Health and Social Care, University of Hull; Kathy Radley is a lecturer in skin health and dermatology care at the Faculty of Health and Social Care, University of Hull, and clinical nurse specialist, dermatology at United Lincolnshire Hospital Trust. (Aged Care New Zealand, Issue 01 2022, pg. 82/83) Comments are closed.
|
AuthorShonagh O'Hagan Archives
July 2024
|

 RSS Feed
RSS Feed